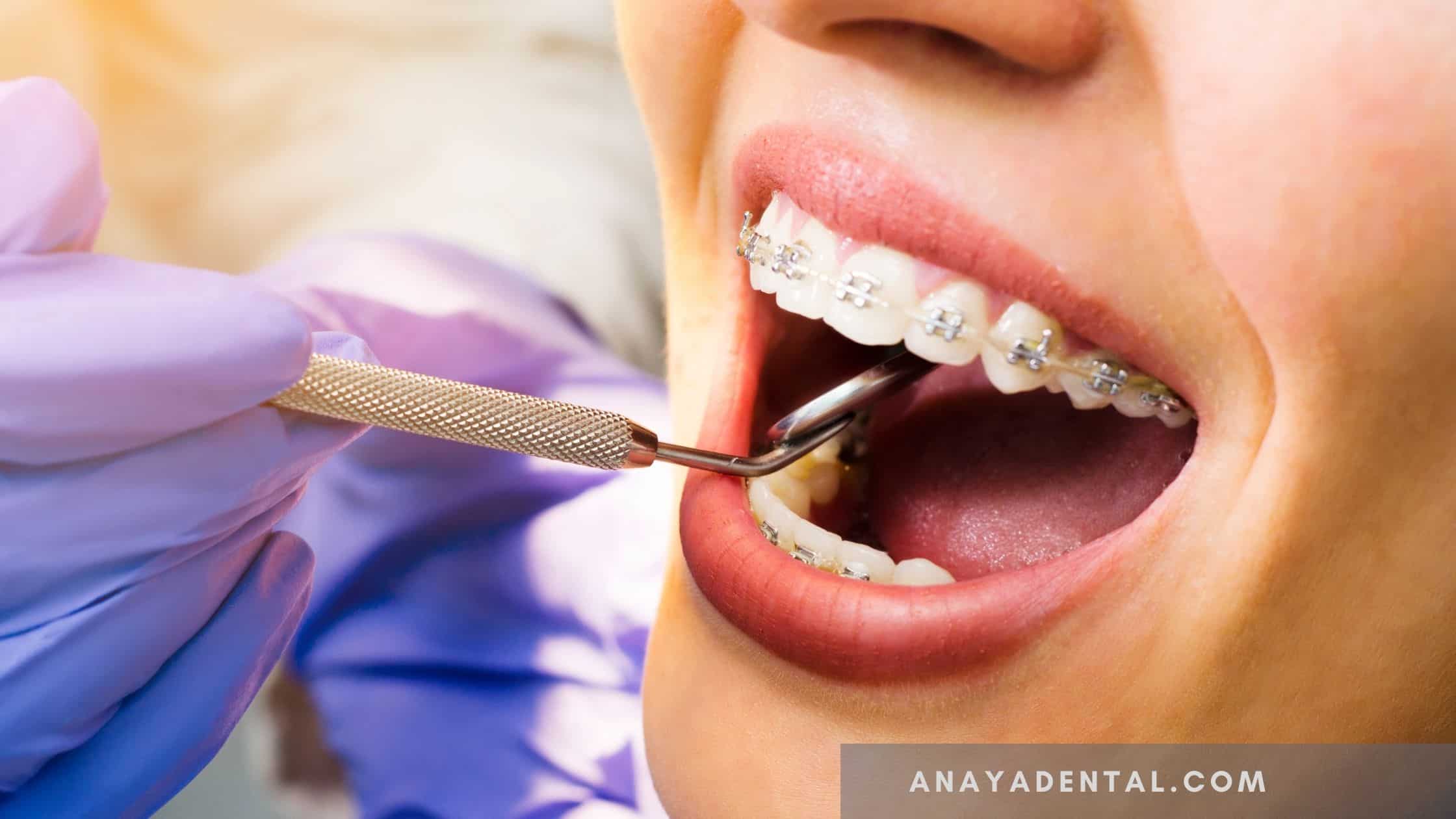
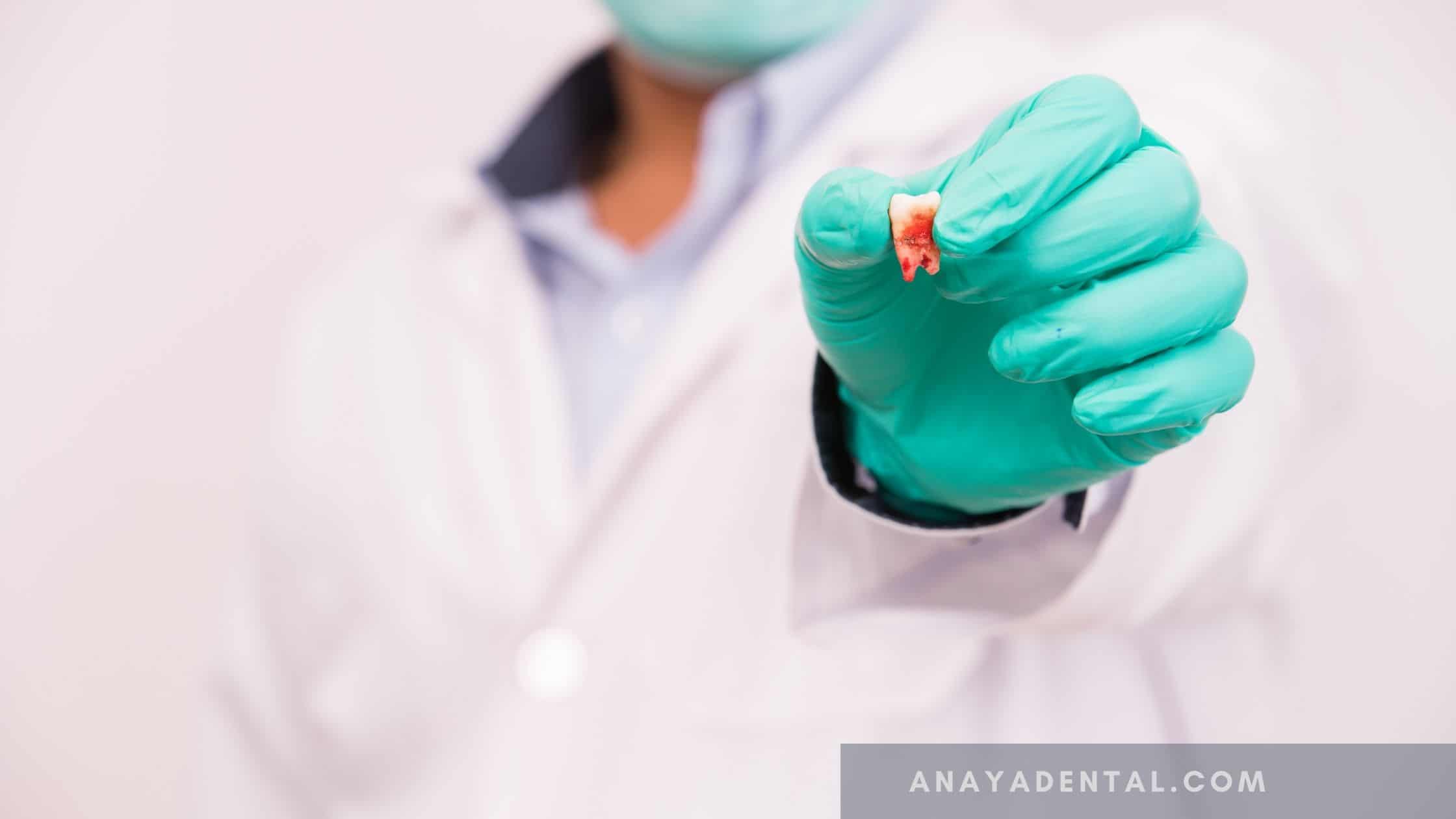
Surgical procedures are always prone to complications whether it’s a major or a minor procedure. Complications during third molar surgery can be divided as follows-
DURING THE PROCEDURE
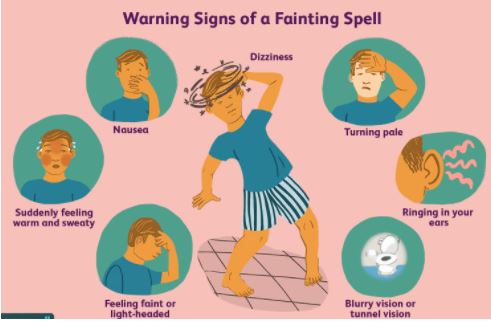
Syncope
One of the most common complications of the procedure. Causes can be numerous but mainly results due to decreased oxygen supply to the brain because of pooling of blood into arms and legs. This situation arises due to increased anxiety and fear in apprehension of the procedure. Hence patients should be well familiarized before the procedure with the whole treatment protocol.
Adjacent tooth luxation
Adjacent tooth luxation can occur when the tooth is taken as fulcrum rather than bone for luxation of molar
Try Our Dental Calculators
Tooth fracture
Tooth fracture can occur due to undesirable force application and incorrect angulation. Ankylosed teeth are most prone to fracture during luxation
Fracture of alveolar process
Alveolar process can fracture when extraction movements are awkward or abrupt. If there is ankylosis of tooth in the alveolar process it can lead to alveolar process fracture.it is most commonly seen in extraction of Canines. Significant problems occur if lingual plate is fractured during molar extraction due to injury to lingual nerve
Soft tissue injury
It occurs most times due to the inept or inadvertent manipulation of instruments (e.g., slippage of elevator) during the removal of teeth. The areas most often injured are the cheeks, the floor of the mouth, the palate, and the retromolar area. In cases with reduced mouth opening soft tissue injury can occur due to excessive force application and prolonged retraction. Tearing of flap can occur during reflection and can also lead to injury to gingiva.
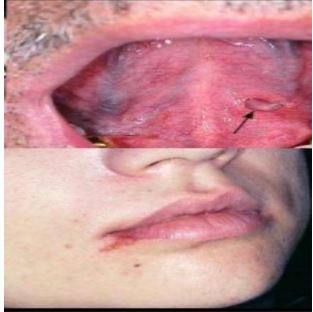
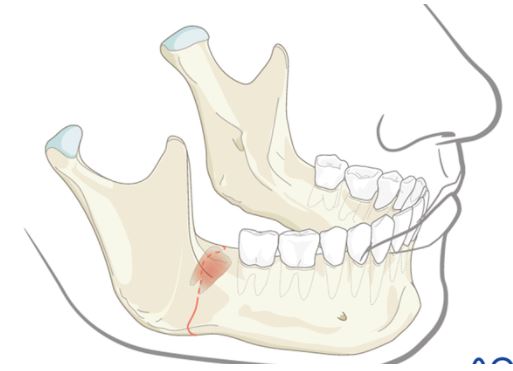
Mandible fracture
Although the chances are very rare yet there are some cases reported for mandible fracture during extraction. Most commonly seen during mandibular third molar disimpaction.
May occur when:
- Excessive force when proper pathway for removal has not been created
- Excessive force on deep roots
- Excessive force on ankylosed tooth
- Atrophic mandible
- Associated Pathology
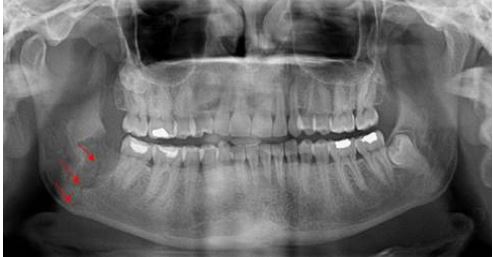
Anatomy variation
Bone form and shape varies from person to person causing difficulty in injecting drugs to correct location.
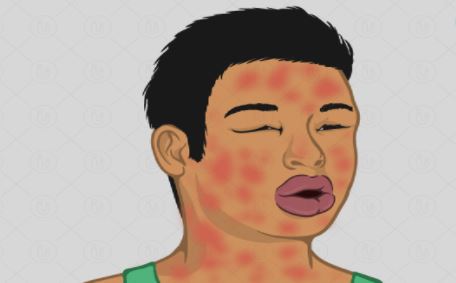
Anaphylactic shock
It is a severe form of allergic reaction to local anesthetic drugs injected to numb the tissues. Though the incidence is very rare but prior testing is a must before injecting the drug
Haemorrhage
Tooth extraction is a stringent test for the haemostasis and coagulability of blood. It is not uncommon for persons without bleeding disorders to report bleeding from socket area. Intraoperatively bleeding can occur due to damage to any of the major blood vessels supplying the area. Firm pressure is applied and suturing is done to arrest bleeding. Hence a routine lab blood workout is a must to prevent such complications.
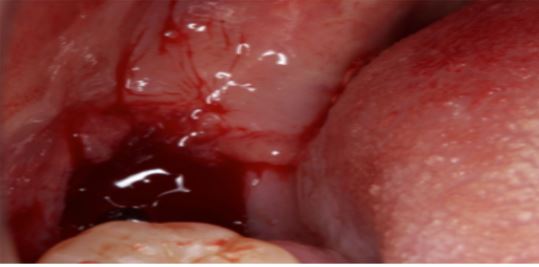
Oroantral communication /fistula
`
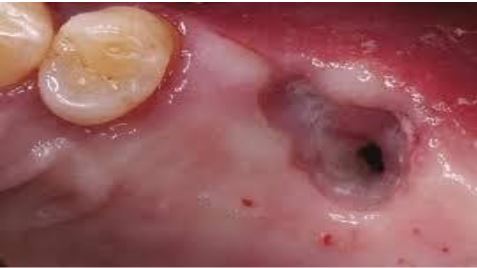
Maxillary posterior teeth having close proximity to sinus lining are prone to oroantral fistula formation during extraction. what is an oroantral fistula??? …..Maxillary posterior teeth are in close proximity to maxillary sinus lining. Sometimes during extraction due to inadvertent manipulation, varied anatomic roots/pathology communication gets established between oral cavity and sinus through extraction socket this is termed as oroantral fistula. Small communications usually close by normal soft tissue healing while larger ones require surgical treatment.
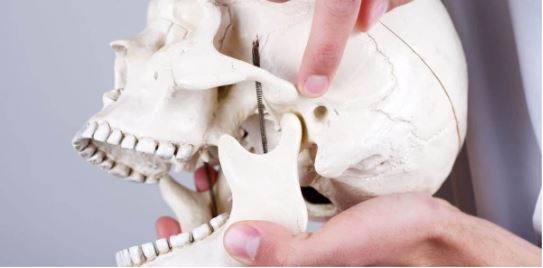
Dislocation of temporomandibular joint
Dislocation can occur readily in the lower jaw during extraction. Patients with history of recurrent tmj dislocation should be managed with well support to lower jaw during extraction procedure. Once occurred it should be reduced immediately as delaying can cause spasm in muscles which can make reduction very difficult.
POST EXTRACTION COMPLICATIONS
Some of the most common post extraction complications are as follows:–
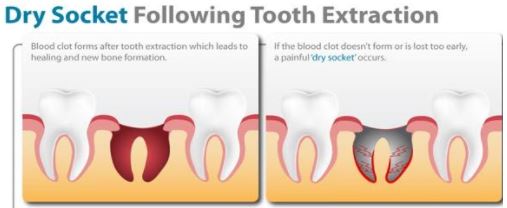
DRY SOCKET
Dry socket has” troubled dentists ever since the practice of exodontia began”. It is one of the most perplexing post extraction complications. WHAT IS DRY SOCKET …
It is a term generally used to refer to delayed onset acute pain in an empty socket area due to loss of blood clot. To read in detail about dry socket click on dry socket.
Post operative haemorrhage
Site of a patient with blood stained dribbling and fury of anxiety is not a relatively uncommon complication. The oral cavity should be cleaned thoroughly removing all the clots but not from the socket area. Making the patient sit down quietly and biting firmly on the gauze placed upon the bleeding socket area will help in tackling the situation.
If bleeding still persists then the socket should be packed with local hemostat dressing e.g. gelfoam and suturing is done. Patient is asked to bite firmly on gauze soaked with local anesthetic containing vasoconstrictor placed on the socket area. Patient should be checked for any blood coagulation disorder or intake of oral/systemic anticoagulants e.g. Apixaban (Eliquis),Dabigatran (Pradaxa),Edoxaban (Savaysa),Enoxaparin(Lovenox), Heparin.
Temporomandibular joint dislocation
Can wisdom tooth cause tmj disorder??….no wisdom tooth doesn’t cause TMJ disorder neither getting them removed. It’s just a complication that can occur during tooth removal and can occur with any posterior tooth irrespective of wisdom tooth. Prolonged mouth opening, excessive retraction force applied, muscle spasm can lead to tmj disorders. Dislocated tmj should be reduced as soon as possible to avoid muscles going into spasm and further complications. Sometimes erupting third molars can cause referred pain to tmj but pain subsides with eruption of tooth.
Frequently asked questions
Does wisdom tooth cause headache
Toothache causing headache and eye pain is one of the common presenting features of wisdom tooth eruption. Pain due to the eruption of third molars can be referred to the ear , jaw bone and the temple region.
Upper and lower jaws, side of head, eye, and ear are all supplied by branches of the trigeminal nerve. Hence pain gets referred from one area to another due to close nerve supply. Toothache and headache on one side are usually due to gum inflammation in the erupting wisdom tooth area accompanied by food debris and bacterial accumulation.
Can a rotten tooth cause headaches……..certainly yes. As bacteria ingress deep into tooth and jaw bone through rotten tooth, nerve endings get inflamed causing referred pain to head along with ear.
In normally erupting wisdom tooth Pain subsides on its own after tooth eruption but you should consult an oral and maxillofacial surgeon for proper evaluation of eruption path, tooth decay or any underlying pathology. Headache can also occur after wisdom tooth removal due to referred pain from the healing socket area. Pain usually subsides in 2 or 3 days, in case of prolonged pain you should always report to your dentist for a review.