Root canal therapy, also called endodontic therapy, is a treatment used to save teeth that have been damaged by decay or infection. The goal of the procedure is to clean out the infected or damaged pulp from inside the tooth so that it can be saved. In many cases, root canal therapy can allow a person to keep their natural tooth rather than have it extracted. The procedure is typically done by a dentist or endodontist, and usually takes one or two visits to complete.
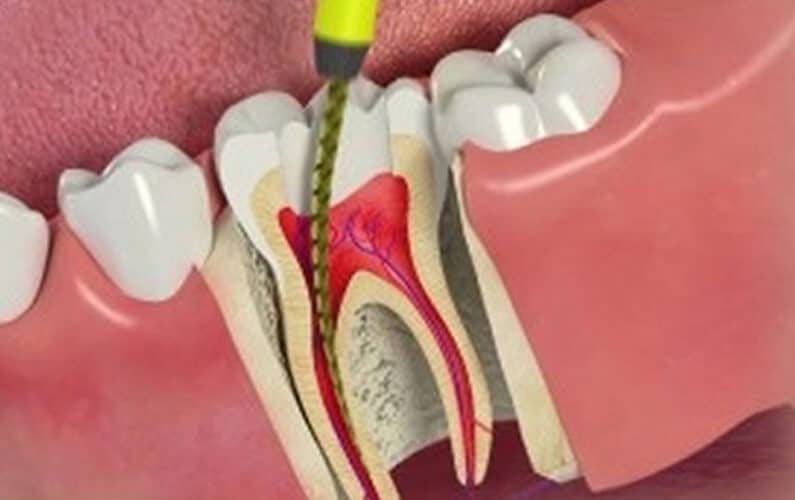
Root canal therapy is generally considered to be a safe and effective treatment, but as with any medical procedure, there are some risks and potential complications that can occur. These include infection, pain, and damage to the tooth. In some rare cases, the root canal treatment may not be successful and the tooth may need to be extracted.
Try Our Dental Calculators
If you are considering root canal therapy, it is important to discuss all of the risks and benefits with your dentist or endodontist so that you can make an informed decision about whether or not the procedure is right for you.
Root canal therapy is a dental treatment that saves teeth from being extracted. When the pulp inside a tooth becomes infected or dies, root canal therapy removes the infected tissue and replaces it with a rubber-like material. This restores the health of the tooth and prevents infection from spreading to other parts of the body.
How do you know if you need a root canal?
A root canal is needed when the pulp inside your tooth becomes infected. The pulp is the soft tissue inside your tooth that contains blood vessels and nerves. If the pulp becomes infected, it can cause a lot of pain and swelling. A root canal is also needed if there is a lot of decay in your tooth.
You may need a root canal if you have:
– Severe tooth pain that doesn’t go away
– Sensitivity to hot or cold temperatures that lingers long after the stimulus is gone
– Swelling or tenderness in your gums
– A tooth that is discolored or has darkening
– A small, pimple-like bump on your gums near the affected tooth
If you have any of these symptoms, you should see a dentist right away. They will be able to determine if you need a root canal and help you get relief from your pain.
STEPS OF ROOT CANAL TREATMENT
A root canal treatment is necessary when the pulp, or blood supply, of a tooth becomes infected. This can happen due to decay, a cracked tooth, or an injury. Once the pulp is infected, it needs to be removed to save the tooth. Root canal treatment is done in different steps:
a) Diagnostic and preparation-
The first step is to take an X-ray of the tooth to see how far the infection has spread and is to prepare the tooth for the root canal treatment.
b) Use of local anesthetics on the tooth–
The most common types of local anesthetics used to numb the teeth are lidocaine and bupivacaine. The dentist will usually inject these drugs into the gums near the tooth that is going to be worked on. The local anesthetic will block the nerves in the area, numbing it so that you will not feel any pain during the procedure.
c) Cleaning and shaping the root canal-
The next step is to clean the root canal. This is done by removing all the debris and infected material from the canal. This can be accomplished with special instruments and irrigating solutions.
Shaping the root canal is a critical step in endodontic treatment as it determines the success of the procedure. There are different ways of shaping the root canal, and each has its own advantages and disadvantages.
One of the most common methods is hand filing. This involves using a hand file to gradually enlarge the canal until it reaches the desired size. The advantage of this method is that it is relatively easy to learn and control. However, it can be time-consuming, and there is a risk of over-enlarging the canal, which can damage the tooth.
Another common method is rotary instrumentation. This uses a handpiece with a rotating cutting tool to enlarge the canal. It is generally quicker than hand filing, but it can be more difficult to control and there is a risk of instrument breakage.
Ultrasonic root canal shaping is another option. This uses sound waves to vibrate a cutting tool and remove tissue. It is generally quick and effective, but there is a risk of damaging the tooth if the ultrasonic waves are not used correctly.
Endodontic procedures can be complex, so it is important to choose a method that is best suited to your individual case.
Alongwith instruments, the use of irrigating solutions has been shown to improve the quality of root canal treatment. Different solutions have been studied, and each has its own advantages and disadvantages. The most commonly used solutions are sterile water, saline, and chlorhexidine.
Sterile water is the simplest solution and is often used as a control in studies. It is effective in removing debris and bacteria from the root canal, but does not have any antimicrobial activity.
Saline is another common solution that is similar to sterile water in terms of its effects.
Chlorhexidine is the most commonly used antimicrobial solution and has been shown to be effective in reducing the number of bacteria in the root canal. It is important to note that chlorhexidine should not be used as the sole irrigating solution, as it can lead to resistance.
The use of irrigating solutions is an important part of root canal therapy. Each solution has its own advantages and disadvantages, so it is important to select the right one for each individual case.
d) Filling the root canal-
Once the root canal is clean, it needs to be filled. This is done with a material called gutta percha. Gutta percha is a rubber-like substance that seals the canal and protects the tooth.
e) Sealing the tooth-
The final step is to seal the tooth. This is done by placing a crown, or cap, over the tooth. The crown protects the tooth and restores it to its original shape and function.
What is endodontic retreatment?
Endodontic retreatment is a dental procedure that is used to correct a number of problems that can occur in the root canal system of a tooth. These problems can include: incomplete healing, recurrent infections, and perforations or fractures in the root. The goal of endodontic retreatment is to save the tooth and prevent further damage to the surrounding tissues.
Endodontic retreatment is often necessary when a root canal procedure has failed or when there has been a change in the health of the tooth that makes it unable to heal properly. In some cases, endodontic retreatment may be used to improve the cosmetic appearance of a tooth.
Endodontic retreatment is a complex procedure that should only be performed by a qualified dentist or endodontist. The success of the procedure depends on many factors, including the experience of the dentist, the type of problem being treated, and the overall health of the tooth.
Endodontic retreatment can be a lengthy and costly procedure, but it is often the best option to save a tooth that would otherwise need to be extracted. If you are facing the possibility of endodontic retreatment, be sure to discuss all of your options with your dentist so that you can make the best.
There are a few different instruments that are commonly used in endodontic retreatment.
The first instrument is called a rotary file. This is a small, hand-held drill that is used to remove the filling material from the root canal. The rotary file is also used to enlarge the root canal so that it can be cleaned more effectively.
The second instrument is called a reamer. This is a larger drill that is used to remove the infected tissue from the root canal. The reamer also enlarges the root canal so that it can be cleaned more effectively.
The third instrument is called a curette. This is a small, hand-held instrument that is used to scrape away the infection from the root canal.
The fourth instrument is called an endodontic file. This is a small, hand-held file that is used to smooth the inside of the root canal.
The fifth instrument is called a ultrasonic cleaner. This is a machine that uses sound waves to clean the inside of the root canal.
Post operative pain after Root canal therapy
Assuming that you have a basic understanding of what a root canal is, we’ll now focus on the post-operative pain that can occur after the procedure. As with any surgery, there is always the potential for some degree of discomfort afterwards. However, this is usually mild and temporary, subsiding within a few days. There are a few things you can do to help manage any pain you may experience.
First, it’s important to take the pain medication prescribed by your dentist or endodontist as directed. This will help to keep any discomfort under control while your body heals. You can also apply a cold compress to the outside of your mouth for 20 minutes at a time to help with any swelling. Finally, be sure to eat soft foods and avoid chewing directly on the treated tooth until it has fully healed.
If you experience any severe pain, persistent swelling, or unusual symptoms, be sure to contact your dentist or endodontist right away. With proper care, your root canal should provide relief from your tooth pain and help you keep your natural tooth for years to come.
Outcome and prognosis of root canal therapy
Root canal therapy is a dental procedure that saves teeth from being extracted. When the pulp inside a tooth becomes infected, the infection can spread to the bone and other tissues around the tooth. Root canal therapy removes the infected pulp, cleans and seals the root canal space, and replaces the lost tissue. After treatment, most people have no problems with their teeth and can expect to keep them for a lifetime.
In some cases, the infection may return or new problems may develop. If this happens, you may need additional treatment. In most cases, however, people who have had root canal therapy can expect to keep their teeth for a lifetime.
Systemic issues related to root canal therapy
Root canal therapy is often seen as a last resort treatment for teeth that are severely damaged or infected. However, this treatment can come with many risks and side effects, such as pain and inflammation. It’s important to weigh the pros and cons of this treatment before deciding if it’s right for you.
Systemic issues related to root canal therapy include:
– Pain and inflammation: Root canal therapy can be very painful, especially if the tooth is infected. The procedure involves drilling into the tooth to remove the infected tissue. This can cause inflammation and swelling.
– Risk of infection: There is a risk of infection when root canal therapy is performed. The risk is higher if the tooth is infected.
Root canal therapy is a treatment that should be considered carefully. The risks and side effects should be weighed against the benefits of the treatment. If you have any questions, be sure to ask your dentist or oral surgeon.
Alternatives of root canal therapy
There are a few alternatives to root canal therapy, including:
-Extraction: This is the removal of the tooth.
–Dental implants: This is a surgical procedure in which an artificial tooth is placed into the jawbone to replace a missing tooth. For this first we have to extract the infected tooth.
-Dental bridge: This is a false tooth that is held in place by being attached to the teeth on either side of the gap. This option is also considered after removal of infected tooth.
FREQUENTLY ASKED QUESTIONS-
1. DOES A ROOT CANAL THERAPY HURT?
A root canal therapy may cause some discomfort during the procedure, but it is generally not a painful experience. The majority of patients report feeling only minor pressure or no pain at all during the treatment. After the procedure, you may experience some tenderness or soreness in the treated tooth, which can be alleviated with over-the-counter pain medication. If you have any concerns about discomfort during or after your root canal therapy, please don’t hesitate to ask your dentist or endodontist.
2. Can I go to school or work after getting a root canal?
Yes, you can go to school or work after getting a root canal. The procedure itself is not very long, and you will likely only experience some minor discomfort afterwards. You should be able to return to your normal activities the same day.
3. What are the risks of not getting a root canal?
If you don’t get a root canal when it’s necessary, the tooth can become infected. This can lead to pain, swelling, and/or abscesses. In severe cases, the infection can spread to other parts of the body, which can be life-threatening. It’s important to get a root canal as soon as possible if your dentist or endodontist recommends it.
4. What are the risks of getting a root canal?
The procedure is typically very successful, and complications are rare. While root canals are generally safe, there are a few risks associated with the procedure.
First, there is a small chance that the infection could spread to the bone surrounding the tooth. Additionally, the tooth could become re-infected if the seal around the filling is not strong enough.
Finally, there is a risk of damage to the nerves surrounding the tooth, which can lead to pain or numbness in the tooth. While these risks are rare, it is important to discuss them with your dentist before having a root canal.In some cases, the root canal may need to be repeated if the initial treatment is not successful.
5. What should I expect after getting a root canal?
You can expect some pain and swelling after getting a root canal. The pain will likely go away within a few days, but the swelling may last a bit longer. You should avoid eating crunchy or hard foods until the numbness in your mouth has worn off. Additionally, you should avoid smoking and drinking hot liquids until your mouth has healed.
You may also experience some sensitivity to cold or hot temperatures for a few weeks after the procedure. This is normal and should resolve on its own. If it does not, or if you have any other concerns, be sure to follow up with your dentist.
6. How does endodontic treatment save the tooth?
Endodontic treatment, also known as a root canal, can save a tooth that is infected or damaged. The procedure involves removing the damaged tissue, cleaning the inside of the tooth, and then filling it with a special material. This helps to restore the function and structure of the tooth so that it can be saved. In some cases, a crown may also be placed on the tooth to further protect it.
7. Cost of root canal therapy
Root canal therapy is a common dental procedure that is used to treat infections in the tooth pulp. The cost of a root canal can vary depending on the severity of the infection, but it is typically a less expensive option than having the tooth pulled.
The price of a root canal will also depend on whether you have insurance. If you do have insurance, your policy may cover part or all of the cost of the procedure. However, if you don’t have insurance, you may be responsible for the entire cost of the root canal, which $500-$2000.
While the cost of a root canal may seem high, it’s important to remember that this procedure can save your tooth from being extracted. In most cases, a root canal is the best way to treat an infection in the tooth pulp and prevent further damage to your smile.
8. Implant therapy versus endodontic therapy
Implants and endodontics are two different dental treatments. Both have their pros and cons, which can make it difficult to decide which treatment is the best option for you. In this article, we will compare and contrast implants and endodontics, so that you can make an informed decision about which treatment is right for you.
Implants are a surgical procedure in which a metal rod is inserted into the jawbone to serve as a replacement for a missing tooth. The metal rod fuses with the jawbone over time, and a false tooth is then attached to the metal rod. Implants are considered to be a very strong and durable option for replacing missing teeth. However, they are also the most expensive option, and the surgery can be quite invasive.
Endodontics is a nonsurgical procedure in which the root canal of a tooth is cleaned out and sealed. This procedure is necessary when the pulp of the tooth becomes infected. Endodontics can save an infected tooth from needing to be extracted. However, there is a small risk that the infection could come back, and the tooth could still eventually need to be extracted.
So, which treatment is right for you? If you are missing a tooth, and can afford it, implant surgery may be the best option for you. However, if you have an infected tooth, endodontics may be the better choice. Talk to your dentist about your options to decide which treatment is right for you.




